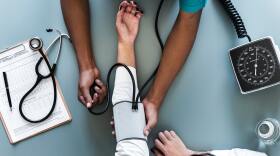
Hospital custodians and houskeeping staff say that even though they clean the COVID wards and are in the room with patients, they aren't given adequate personal protective equipment. Three people we spoke with said because it is commonly known among other hospital staff that the sanitation workers are more exposed to the virus, they are treated unfairly and subject to discrimination.
One source, who wished to remain anonymous, cried as she talked about being barred from the lunch and kitchen area she's been accustomed to using, and looking inside and seeing doctors and nurses she'd been working with all day.
That means she works hungry, she said, as custodial staffers are not allowed to eat wherever they want to in the hospital—she can eat while she's standing or walking, but she can't sit down with a lunch.
She also spoke of how sad her job has become, watching COVID patients die alone, without their families, and how sometimes she's the person these patients talk to as their health deteriorates.
When families come to Albuquerque from other parts of the state because a loved one needs care at the hospital—something that's happening a lot during the pandemic because many of the intensive care beds are here—they often don't have a place to stay, she said, so she lets them stay at her home.
She speaks primarily Spanish, and she was interviewed by reporter Yasmin Khan, who also spoke with and translated interviews with two other members of the cleaning crew at the University of New Mexico Hospital:
Delmy Nova and Alicia Hernandez are part of the cleaning staff at UNMH. Nova works in urgent care, cleaning rooms that receive a range of patients. Hernandez works on the second-floor surgery ward and is also a union delegate for the cleaning staff. Neither are speaking on behalf of the hospital, but only sharing their personal experiences. The women say things have changed drastically for them in terms of their mental and physical health since the pandemic hit, in part because they haven’t received training on how to deal with the virus at work.
Nova says the first days of the pandemic were rough, and things haven’t gotten better.
“It was chaos," she says. "It was total panic because it was something unknown to us and we didn’t know how to confront this virus. We are still in the same situation because we still don’t know how to respond. We are using the tools we have but we are really limited.”
Hernandez says about 80 percent of the cleaning crew are women. She says some staff assigned to clean rooms with coronavirus patients have pre-existing conditions that make them more susceptible to COVID-19 complications if they contract the virus. However, even with doctors notes, she says high-risk staff are still asked to clean rooms with COVID-19 patients. “They are obliging workers with pre-existing medical conditions to enter COVID-19 contaminated rooms exposing workers without listening to the worker’s doctors or taking pre-existing conditions into consideration. The life of our colleagues is important, the health of our colleagues.”
The women say they are also concerned that they didn’t receive information or training in how to use the new cleaning supplies they received this week. Without understanding how to use the new chemicals correctly, they are afraid they are putting themselves, patients and other hospital staff at risk.
Both staff members say they knew the old solution, Virex, worked to kill the COVID-19 virus within 1 minute, but they don’t know how long the new solution takes to work, and since they enter dozens of rooms per day, they feel exposed to the virus. They also say they don’t have the right PPE, and since they are working in rooms with coronavirus patients, they need more than a regular surgical mask. They want N95 masks that are more effective against the virus.
Neither women say they have had luck talking with their supervisors about their concerns.
Nova says she understands doctors and nurses are in close contact with patients and are at high risk for contracting the virus, but cleaning crew are also exposed and deserve the right PPE, hazard pay and to know how to correctly use the new cleaning chemicals. “The doctors and nurses are important for the hospital, and we are too. If we aren’t there to clean and sanitize the rooms for patients, then they couldn’t do their job 100 percent. The virus will affect a cleaning staff just as much as a doctor. It doesn’t discriminate. It attacks everyone.”
Both women say the lack of PPE leads to emotional stress because doctors, nurses and other staff avoid them—similar to the first woman’s experience of being barred from eating in the lunchroom with other staff. “I see that doctors and nurses pass each other normally in the hall, but when they pass cleaning staff, I see them panic,” Nova says.
Hernandez says her union has tried to negotiate with CEO Kate Becker of UNMH for hazard pay, better PPE, paid quarantine leave and measures such as taking temperatures of workers when they leave and arrive. But they haven’t had luck reaching hospital administration. “It’s very important that all the listeners know what is happening in UNMH, that we need to reach Kate Becker, the CEO of the hospital, and let her know that the cleaning crew needs her support,” Hernandez says.
The women say because they have children and parents who have medical conditions, they are afraid they are bringing the virus home to their families—especially since they don’t have the right PPE. “Us Latinos," Nova says, "we are very close to our elders. For us, they are people of wisdom, an example of how to live our life. We are proud of them in our hearts, and we love our elders very much, and they often live with us. We live in fear of bringing this virus back to our elders at home.”
Despite all of this, the women say they are proud of their work and they want other cleaning staff around the state to know they can ask for what they need to be safe. “I do my work with pride," Hernandez says, "because the health of others depends on our work. My contribution is beneficial for the hospital, the patients and the staff who work there.”
Nova adds that they have to work—they don't have a choice. “But we also have an obligation to society. For example, my father has cancer. He has Lymphoma, and so I think 'What if my father has to use this hospital room?' So I have to make things right, for my father and for other patients who have serious conditions.”
*****
UNMH spokesperson Mark Rudi did not respond to many of the specific concerns presented by these workers that we sent over via email. This is what Rudi wrote in response:
"We take all allegations of mistreatment seriously, and will look into these claims, but we can tell you that employee and patient safety is our top priority at University of New Mexico Hospital.
As Dr. Steve McLaughlin discussed on KUNM just recently, UHMH has formed a multidisciplinary committee
We work hard to provide venues for all of our employees to share concerns, including weekly town halls, an intranet question and answer forum about COVID-19, and daily employee huddles. We have also held classes that discuss the COVID response and how to stay safe. These concerns have not been brought forward in those platforms, and [hospital CEO] Kate [Becker] has not been approached by any housekeeping employee to discuss these concerns.
We will not tolerate discrimination against any of our employees. We have implemented appropriate social distancing measures in our dining areas, and those measures apply to all employees. We are proud of our housekeeping team and recognize the critical role they play in caring for our patients. We will continue to work to support them."